Dr. Virender Sangwan
Dr. Virender Sangwan is renowned ophthalmic surgeon and innovator in stem cell therapy for corneal blindness, with global impact through translational research, surgical innovation, and leadership in vision care advancement was interviewed by Dr. Soumya Singh, Creative Editor of InnoHEALTH Magazine.
Ortho-K, or orthokeratology, is gaining popularity as a non-surgical way to temporarily correct vision. From a clinical and scientific standpoint, how exactly does Ortho-K reshape the cornea, and who can benefit most from this technique?
The Ortho-K is suitable for low myopes, and it essentially mechanically reshapes the cornea during sleep, and the effect lasts temporarily during the day. This way, people who prefer not to wear spectacles or contact lenses during the day find this technique helpful for short periods.
Are there any long-term risks or widespread misconceptions about Ortho-K that you feel the public should be more aware of?
The only small risk is infection, and other than that, it is largely a safe technique. People should understand that it is not a permanent vision correction.
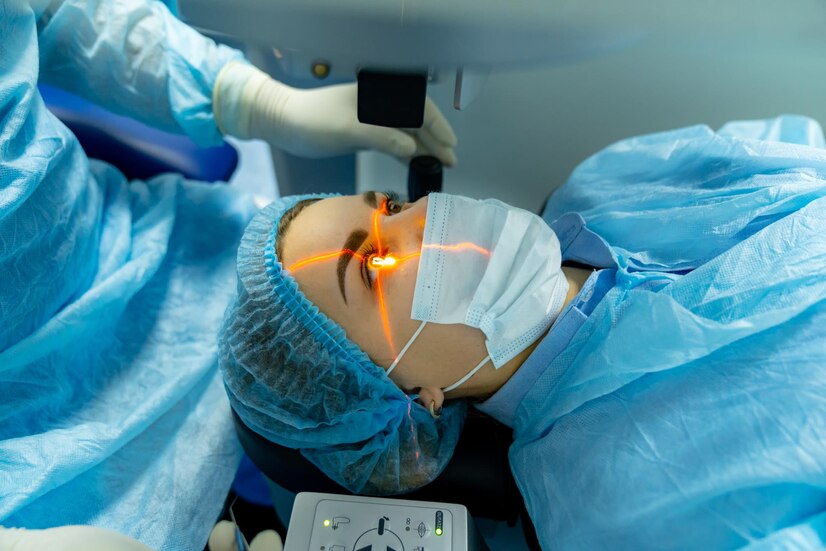
Both LASIK and SMILE are laser-based refractive surgeries. Could you explain the core differences between the two, and under what circumstances one might be preferred over the other?
LASIK means Laser-Assisted In Situ Keratomileusis: it is a type of laser refractive surgery to reshape the cornea for correction of refractive errors like shortsightedness. The SMILE is a type of laser eye surgery to correct refractive errors, and it is a type of LASIK. The SMILE- Small Incision Lenticule Extraction is a minimally invasive and flapless laser surgery. The LASIK can be done using a blade or a non-touch technique like SMILE. There other type of LASIK like PRK or PTK. The technique is decided based on several factors like corneal topography, thickness of the cornea, degree of refractive error or power to be corrected, patient preference etc.
The concept of bionic eyes sounds like science fiction becoming reality. From your vantage point in translational ophthalmic research, how do these devices function, and what potential do they hold for patients with severe visual impairment?
Let us first understand how the eye perceives light or images. The front part of the eye (the Cornea and Lens) collects light and focuses it onto Retina, which in turn sends a signal to the brain via the Optic Nerve. When there is irreversible damage to the retina (retinitis pigmentosa, retinal degeneration, etc) a bionic eye can be useful to partially restore vision. The bionic eye is also known as a prosthesis designed to restore some degree of sight to individuals with severe visual loss. The device consists of external components like a camera and a processor to capture & transmit visual
information. The Argus II retinal prosthesis system is such an example of a bionic eye that has been used to treat individuals with severe retinitis pigmentosa. It includes a camera and an electrode array implanted on the retina.
With your experience bridging clinical practice and research, how do you see artificial intelligence transforming the early detection and diagnosis of diseases like diabetic retinopathy and glaucoma?
The artificial intelligence (AI) in the medical and ophthalmic field is transforming the care, and we are implementing these technologies in our research and patient care quickly. I believe the AI is going to help doctors and patients simplify care and processes.
You’ve spent decades striving to make eye care accessible to underserved populations. What recent advancements in tele-ophthalmology have most effectively extended reach to rural or low-resource communities?
There are few technologies which are helping us to reach the unreachable in rural areas. Yes, using Tele-ophthalmology is one such tool and we are practising it extensively in our daily life. The Dr Shroff’s Charitable Eye Hospital (SCEH) has over 6 secondary center, 125 primary eye care centers in addition tertiary care center in Delhi. We examine over 700,000 patients in OPD, over one million school screenings and perform 78000 surgeries in a year. We have been using technology extensively to make it happen, including tele-ophthalmology and tele-refraction.
Femtosecond laser technology has been a game-changer in both cataract and refractive surgeries. Could you share how this innovation has improved surgical precision and patient outcomes?
The femtosecond laser technology is still evolving and making eye surgery more precise, and not necessarily improved the patient outcome. I think the technology has to improve further to improve patient outcomes yet.
You’ve treated over 800 patients using cultivated limbal stem cells, making it the largest known application of adult stem cell therapy in ophthalmology. What have been the most profound outcomes or challenges from this experience?
I have been using and working with stem cell therapy for corneal blindness from the early 2000s and established for the first time cultivated limbal epithelial transplantation (CLET) and then devised new technique of growing stem cells using the eye as “Petri-dish” and regrow damaged corneal outer layer (called as corneal epithelium). This technique is called SLET-simple limbal epithelial transplantation. We don’t need an expensive laboratory for the SLET, and it is a very cost-effective surgery. There has been a profound effect on patients of using these procedures. We have been able to restore vision in some of my patients who have been blind due to chemical injury for 30-40 years.
Translational research has defined much of your career. How do you see the relationship between lab-based discovery and real-world clinical application evolving in the next decade?
Translational research is the foundation of my 30+ years career, and it continues to define my current work. For this purpose, we have established stem cells research laboratory and also SPCORE- Shroff’s Pandorum Centre for Corneal
Regeneration. We also started a PhD program in translational eye research in collaboration with MAHE- Manipal Academy of Higher Education. We have enrolled five PhD students in this program who are solving actual clinical problems faced by our patients. Therefore, the future lies in translational research to improve patient outcomes.
You’ve worked extensively with institutions like LV Prasad Eye Institute and ORBIS International. What insights have you gained about merging innovation with equitable care, especially in resource-limited settings?
I have always worked in not-for-profit organisations throughout my career. Innovation is the key driver for improving access to healthcare for all, as well as for enhancing clinical outcomes through the participation of all stakeholders in an equitable manner. Technological innovations are more relevant in resource-limited settings. Hence, we have started an innovation centre at L V Prasad Eye Institute in 2013, which was inaugurated by Hon’l APJ Abdul Kallam, then president of India. The centre was named as Centre for Innovation and the program “Engineering the Eye”.